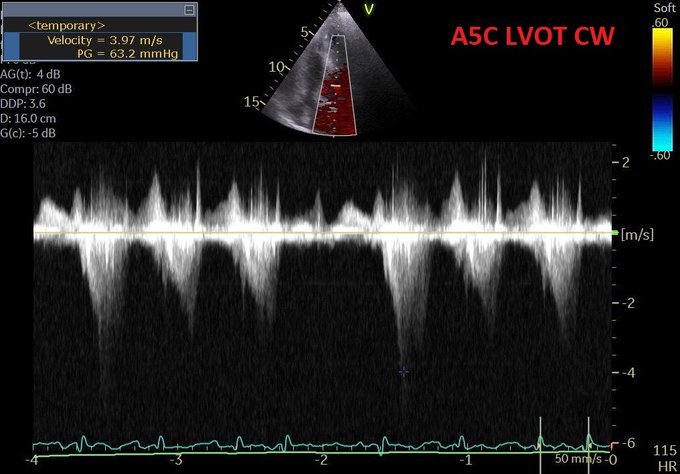
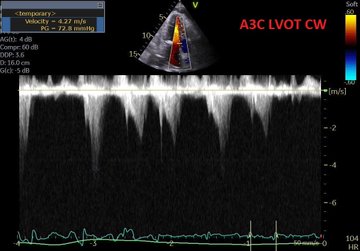
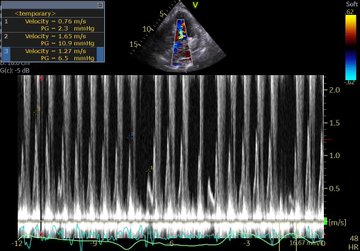
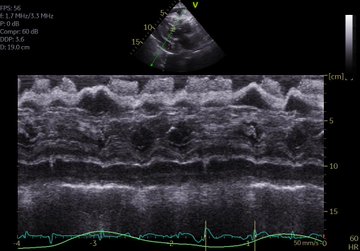
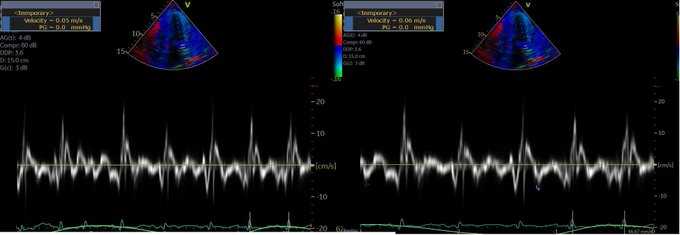
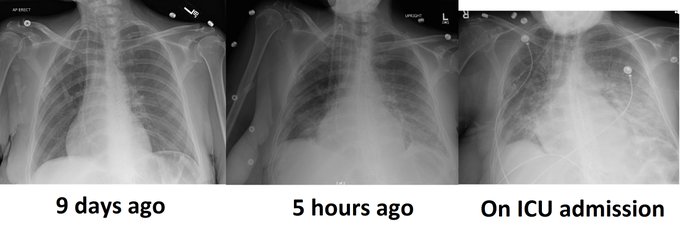
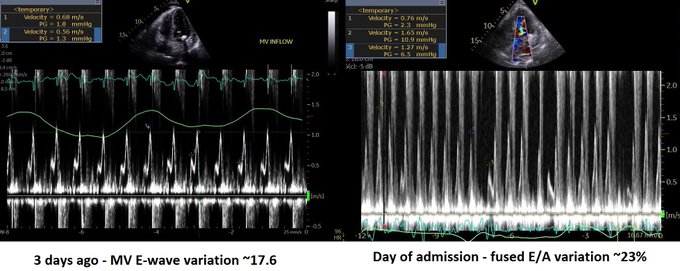
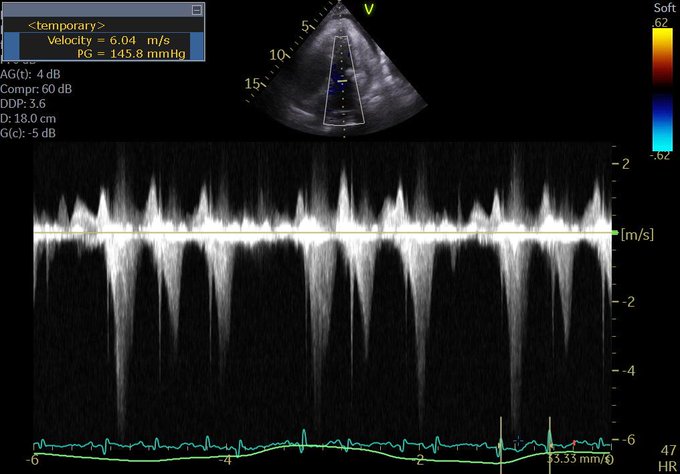
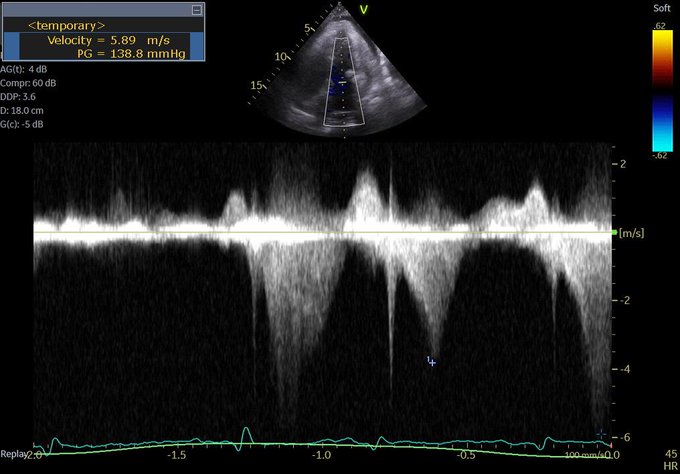
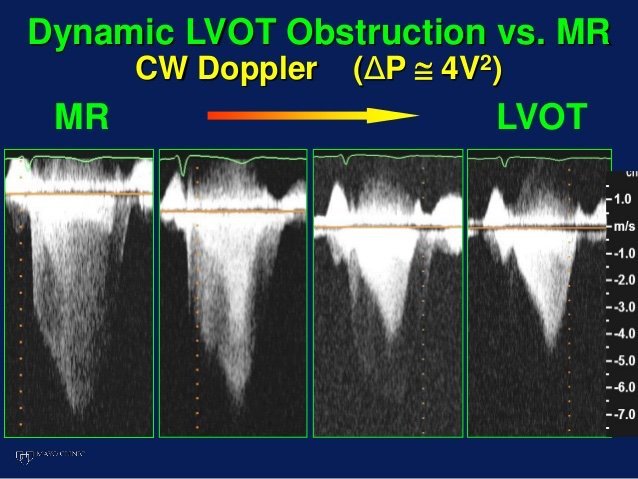
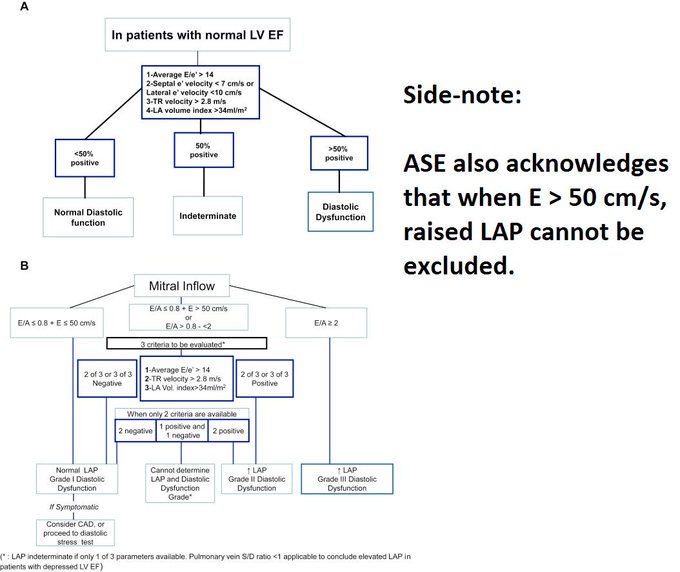
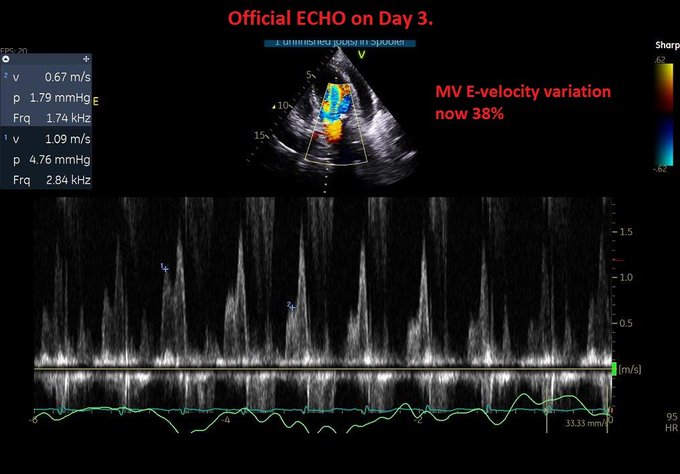
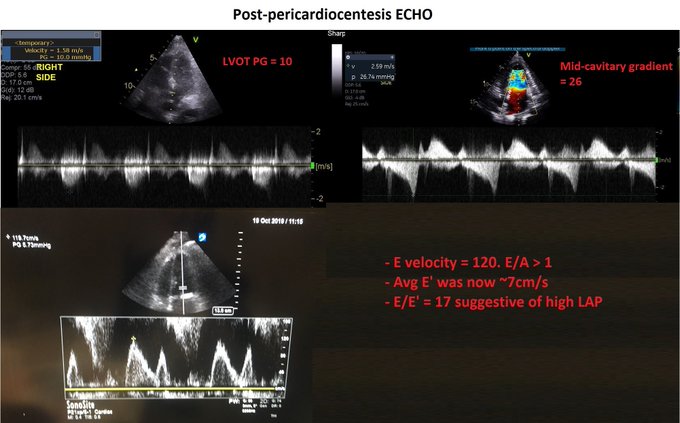
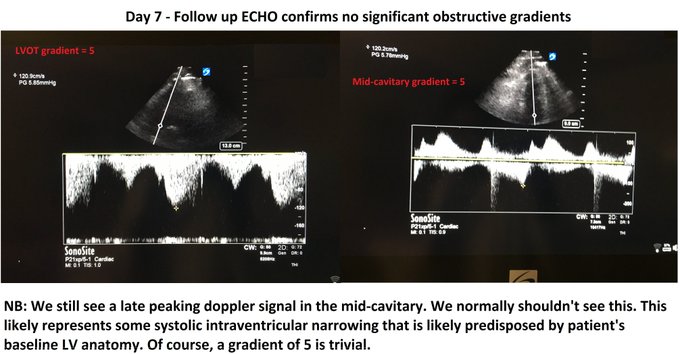
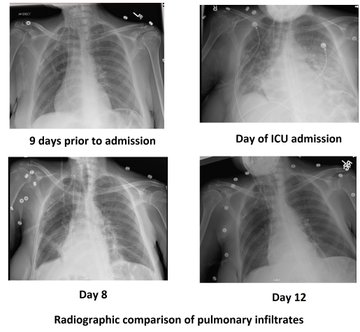
Perhaps this slowed up (0.5x) A3C loop will help with that LVOT doppler!
IVC POCUS
“Volume Status” and other meanderings. #FOAMed, #FOAMcc, #FOAMer #POCUS
So the discussions go on about volume status and POCUS, and recently one in particular made me realize that it is important to reframe the way we think about “volume status.” As Segun Olusanya (better known as @iceman_ex) said, “the IVC is not a fuel tank indicator,” and indeed it is not. But even if it was, would that be useful? If somehow, an 18 mm IVC (short axis circular or average of course!) corresponded exactly to a 0.70 ml/kg blood volume, would that be of any use?
No. Of course not.
I get asked this question in consult a lot. So I could be a stickler on principle and answer, whether verbally or in a consult, that the volume status cannot be precisely ascertained using POCUS, and keep walking down the hospital hallway.
But let’s instead reconsider the true clinical question for a moment. What does “volume status” mean when requested by a colleague. The truth is that he or she is likely asking you whether there is a need to give fluid, remove fluid, or stay the course.
Ahhhh. Now POCUS, the IVC and its friends can help. A lot. A lot more that most clinical examinations and chart reviews of weights or ins and outs can. Way more. Why? Because if you are cool, with a normodynamic heart and a small IVC, you are on the low side of volume. Now you may also have a lot of B lines from your pneumonia and the lack of volume tolerance will give your answer to be very careful with fluids. If you are warm and hyperdynamic with a small IVC and totally clear lungs, no elevated ICP and a soft belly, you may just be vasodilated but, if your BP is on the low side, some fluid is a fair go, so long as you follow closely thereafter for fluid stop points. If you have a low urine output, a big IVC, a pulsatile PV and a poor LV, you probably need lasix, no matter how clear your lungs are and even if your creatinine is rising, in fact, especially since it is rising.
The permutations are myriad. But that’s why we have MDs and are supposed to be able to integrate bits and pieces of physiological data to come up with an understanding of our patients. And POCUS gives us an unprecedented bedside view into this physiology.
So if you do have legit POCUS skills, and are able to do a bit more than a long axis M mode of the IVC, then try this instead:
“Sure thing, now tell me a bit about your patient – I imagine you’re debating whether to give some fluids or diurese?”
Forget about volume status in terms of absolutes. Just think of what the clinical question is, and give your colleagues the answers they need.
I think the patients will do a lot better that way.
I’ve already put up a lot of stuff about the IVC here over the years.
cheers
Philippe
#POCUS IVC Pitfall Twitter Poll & Discussion. #FOAMed, #FOAMer, #FOAMcc
So I ran a couple of twitter polls sets the other day. Here is the first:
(if you want the twitter videos see here)
and part 2:
And to sum it up:
So I just wanted to illustrate something I keep bringing up, essentially that the entire IVC literature based on the AP diameter measurement is physiologically and mathematically flawed. I think the poll and images above clearly support this: given a short axis view, clinicians clearly have a different opinion (and possibly intervention!) than using only a long axis view.
My take, as I’ve said and will keep saying, is that there is a lot of info in IVC POCUS, and the one I am LEAST concerned with is volume responsiveness, which sadly seems to be everyone’s only focus nowadays when it comes to the IVC.
But here’s some food for thought, some of my clinical applications in 5 seconds of scanning:
initial shock patient: big fixed IVC -> no fluids, hurry and find the downstream problem and correct!
resp failure patient: small IVC -> it’s not a massive PE, keep looking for the cause don’t send for a STAT CT angio!
AKI patient: big IVC look at venous doppler and call for lasix, stop the fluids and albumin that were being mistakenly given!
AKI or shock patient & small IVC: sure , start with some fluids and reassess soon (that means hours not the next day)
etc..etc.. there’s more, and “fluid responsiveness” is only in extremes and fairly low on the list for me!
cheers
Philippe
ps if you like physiology, and a physiologico-clinical approach, don’t miss H&R2019!