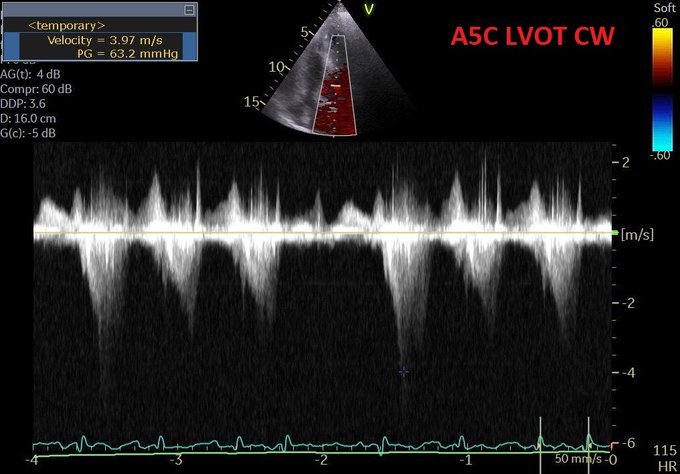
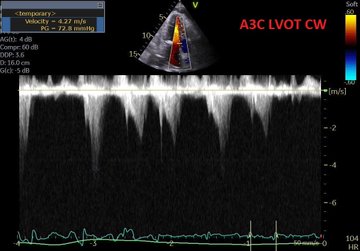
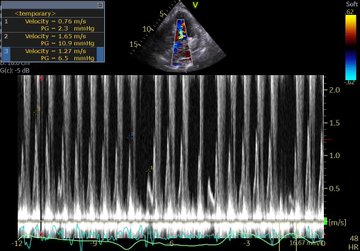
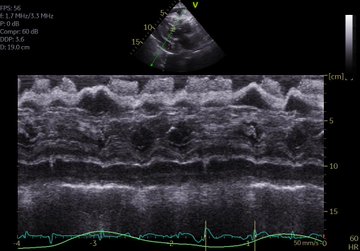
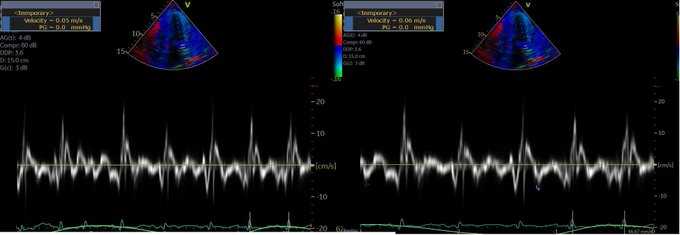
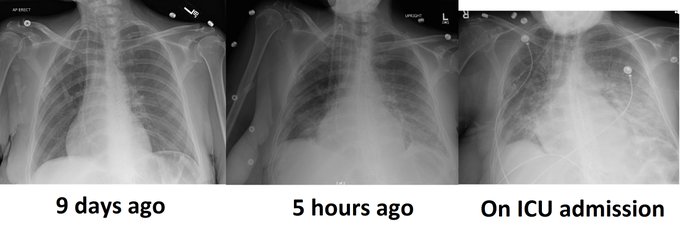
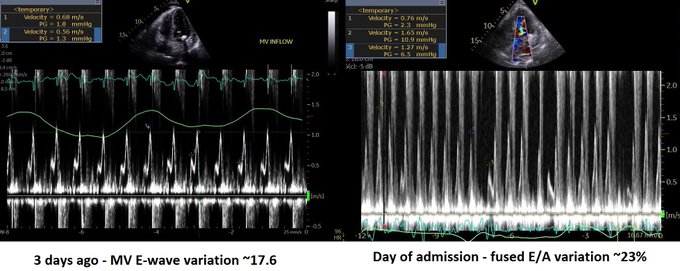
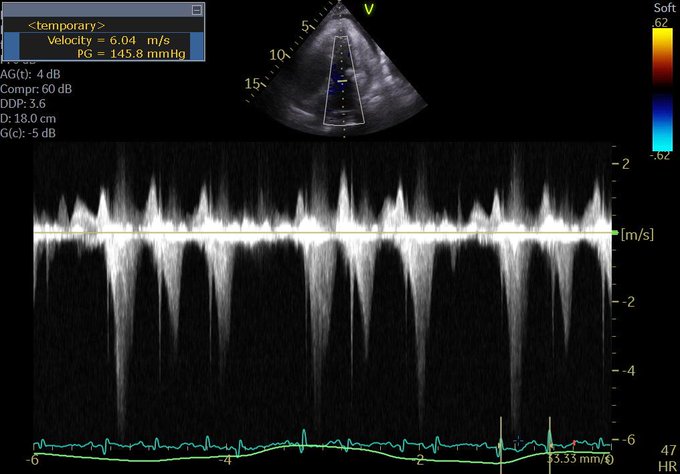
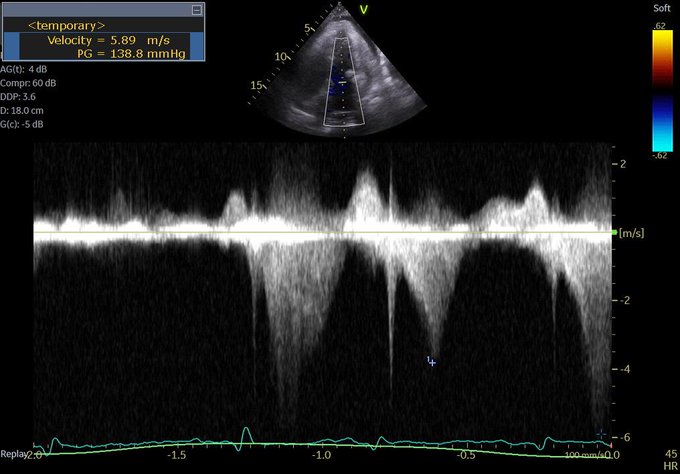
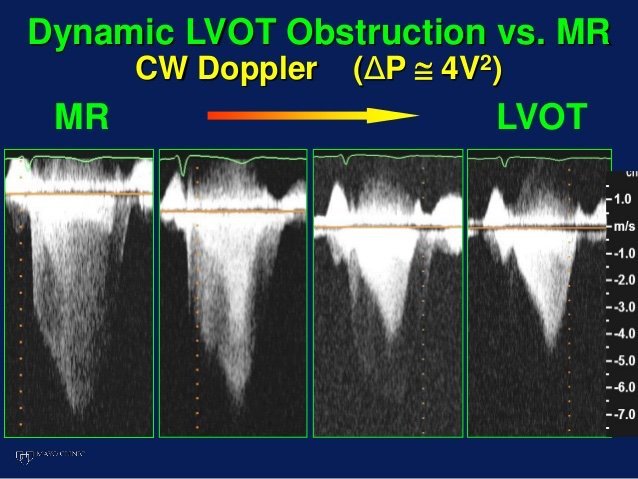
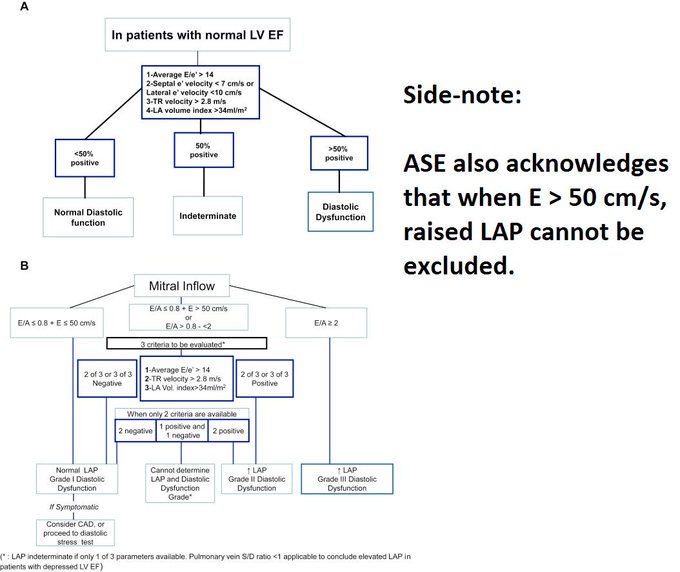
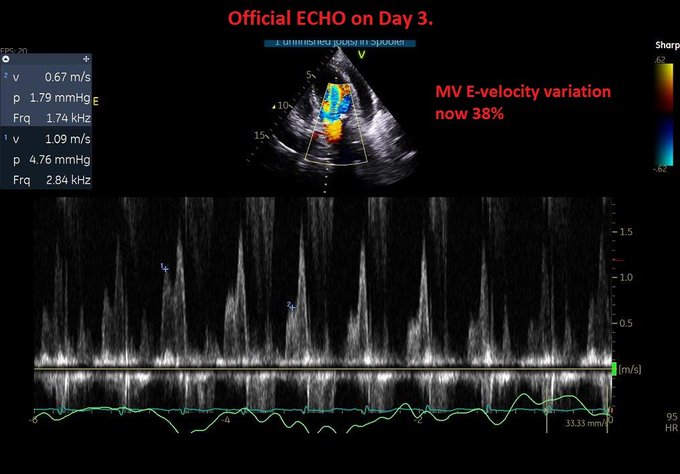
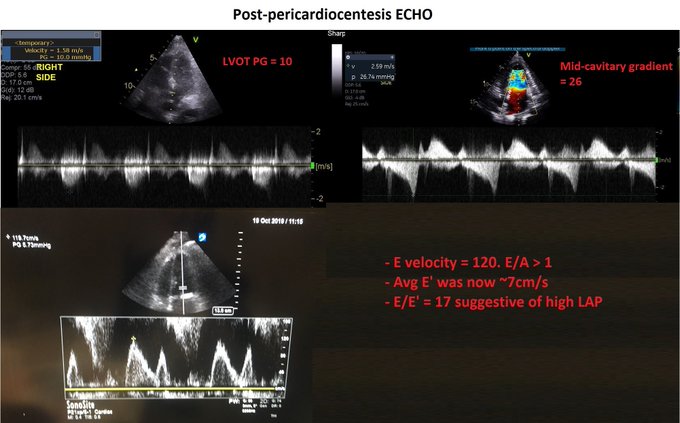
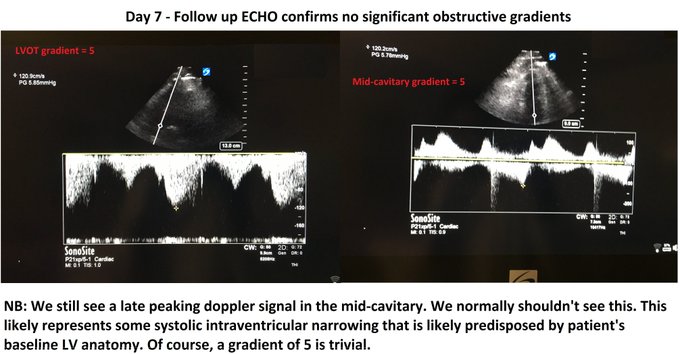
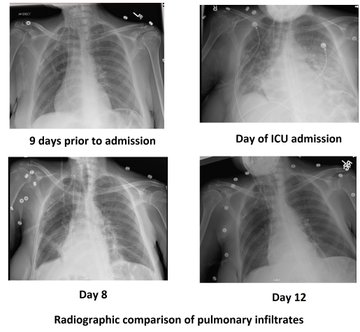
Perhaps this slowed up (0.5x) A3C loop will help with that LVOT doppler!
albumin
The Subtleties of the SHOC-ED Trial: Don’t Just Read The Abstract! #FOAMed
So this was my comment to my friend Jon’s awesome discussion on the SHOC-ED Trial, which is certainly interesting.
Jon, great post as always! I do agree with most of it, but would have to caution readers about reading it with the filtered glasses that make people too often take home the message that they want to – usually the path of least resistance (or change). I think your main point and most critical one is that there is no protocol or recipe that should ever be applied to resuscitation, especially single-variable-based resuscitation (eg old school orders like CVP>12 lasix and <12 bolus), and substituting the IVC for CVP won’t help. And from a standpoint of volume-responsiveness, I totally agree, with the understanding that as the IVC gets more plethoric, the percentage of responsive patients will decrease, inevitably, but one cannot predict with certainty whether that one patient will or will not. However, the parallel change is that, as the IVC gets more plethoric, the volume tolerance is likely decreasing as well, so that your benefit to risk ratio is dropping. And of course you can’t recipe that just based on IVC, but should be looking at the site of pathology (eg lung, brain abcess, pancreatitis with ACS, etc…), physical exam, to determine your patient’s volume tolerance. Because we all know that most of that miraculous fluid will end up clogging the interstitium, with consequences ranging from cosmetic to fatal (though usually blamed on the patient being “so sick” in the first place, absolving the clinician from any wrongdoing). So comments like the one previous to mine, stating “give volume and see if the response occurs” are, in my mind, a poor approach. We know from studies that you cannot simply remove the fluid you gave and go back to the start with lasix (glycocalyx damage, etc), and we also know that much of the effect of said fluid administration dissipates in minutes to hours (I’m sure Jon can quote these studies off the top of his head!).
As we have discussed in the past, I think POCUS is much underused as a fluid stop point – most of its use is on the ‘let’s find a cool reason to give.’ I would argue that you should hardly ever give fluid to a full IVC (especially if markers of pathological congestion are present – portal vein pulsatility and all), unless you are dealing with temporarily improving tamponade or tension pneumo, because even if you are volume responsive, you are likely not volume tolerant. This also goes to the point that a single, initial POCUS exam will potentially not have the same impact as a whole POCUS-based management which will use it to reassess congestion status, cardiac function, etc.
Having said all this, the most important part of the SHOC-ED article is, in my mind, their discussion, which is full of all the important reasons why the final conclusion is not `we don’t need to do POCUS in shock,’ which is what I see happening (similarly to the TTM reaction), as they outline the cognitive fallacy of putting on trial a diagnostic tool whilst the therapeutics are not yet clearly established. Those only reading the abstract or conclusion will actually miss the important points of this study which the authors clearly explain.
In particular, the ‘rare’ instances of tamponade or aortic aneurysm or PE in their series would be diluted out by the sepsis, but for those patients, it would matter. As the authors state:
‘one might argue that even a single unanticipated emergency procedure would justify the use of POCUS in critically ill patients.‘
I would have to wholeheartedly agree.
cheers
Philippe
The Resus Tracks 04: Shock Circulation & Renal Perfusion with Korbin Haycock. #FOAMed, #FOAMer, #FOAMus
So I got to have a chat with ER doc extraordinaire Korbin Haycock today, reasserting my belief that tissue perfusion is not proportional to blood pressure. I am again including the article discussed, and here is the graph in question:
Here is our talk:
And the paper – which is definitely worth a read, as it clearly supports individualizing therapy!
cheers and please jump into the discussion!
Philippe
Kylie & Korbin chime in to the Venous Congestion Issue. #FOAMed, #FOAMcc, #FOAMus
So I think much of the awesomeness of #FOAMed is sparking discussion and exchange, and the many little steps in clinical management besides the initial prescriptions. So I thought I would highlight and exploit a couple of really interesting reader comments:
So first, Kylie (@kyliebaker888):
Great to listen guys, thanks, and very timely. I had just read Tremblay’s paper after coming across a very pulsatile PV in a relatively well elderly patient with bad TR. Two questions – which PV are more likely pulsatile in the first place….Tremblay mentions RVF/TR and very thin folk. What is your experience?
Second Question – what did the GB wall/GB fossa look like after the initial very positive fluid balance? Does everyone blow out their GB wall with fluids, or only some?
It is always important to isolate the patients’ whose physiology may change the clinical signs (in this case PV pulsatility) and make their interpretation different. I agree that massive TR, especially chronic, would likely account for pulsatility. I am not certain about the physiology for the very thin patient, but I have heard the same thing from Andre. So my personal take on a patient with severe TR and a pulsatile PV would be to look at the IVC variation, TR notwithstanding, if it is fixed and plethoric I would diurese – the organs don’t care what the cause of the congestion is.
As for the GB, I have also seen edema, and then try to correlate with cholestatic enzyme changes that would be out of proportion to the hepatocellular enzymes if there is a primary GB process. This is certainly an imperfect science. In a critically ill septic patient, I have a low threshold to drain the GB if in doubt.
Then Korbin gives his two cents, and then some!
Great case, loved it. Thoughtful management, brilliant!
I couldn’t help thinking as I listened, that it is so important to avoid over-resuscitation with fluids in the first place. We all know that the majority of crystalloids given will end up as interstitial edema, so any benefit from the increase in stroke volume is temporary at best (consider carefully what you gain and at what cost). Wet lungs=increased mortality, days on the vent, and ICU stays. Wet kidneys=AKI 2-3 days after initial resuscitation and potential RRT. Congested liver=gut edema and continuation of inflammatory cytokines/sepsis syndrome. Too much fluids–>BNP levels rise, high BNP levels in the presence of LPS=glycocalyx shedding, and more interstitial edema everywhere.
Cannot agree more.
I think there is some decent evidence that an early fluid liberal approach combined with a late fluid restrictive approach can potentially benefit a patient in septic shock, but its clear that an overall positive fluid balance does harm. Perhaps, even the early fluid liberal strategy (in sepsis specifically) should be tempered by a careful consideration of what is really going on.
My take here is that, by using POCUS, there is no need for a “general approach.” POCUS takes essentially no time. In about 5 seconds you can confirm a small IVC that can (initially) take fluid, a medium one (that you need to watch) or a full one (yes, it happens – that gets no fluid). So to me there is no need to have a pre-determined approach…
Sepsis is an entity characterized by venous return being limited by a decrease in mean systemic pressure (MSP) due to an increase in venous capacitance, rather than a decrease in fluids that generates the stressed volume (MSP=fluid filling/venous capacitance). The body compensates with an adrenergic response that maintains (or attempts to maintain) MAP by an increase in a catecholamine driven augmentation in cardiac output/contractility. This adrenergic response likely has more to do with the increase in lactate production observed in sepsis, rather than actual tissue hypo-perfusion and anaerobic metabolism mechanism. Increases in CVP inhibit venous return and congest the kidneys and GI tract (the left atrial pressures are the equivalent problem for the lungs, combined with the fact that pulmonary vascular permeability is increased in sepsis as well). Given this, I think in distributive shock, we should fix the lack of MSP by an earlier vasopressor therapy approach, both to supplement and decrease the crystalloid load to the patient, which is un-natural and contrary to their deranged septic physiology.
Agree.
Also, could the type of crystalloid given be important? NS gives a considerable sodium load compared to LR, and this likely promotes/sustains fluid retention that is difficult to remove during de-resuscitation. The high chloride levels of NS will promote an increase afferent arteriolar vasoconstriction and thus decrease GFR, making it more difficult to diuresis the patient later on, and contribute to AKI beyond the iatrogenic interstitial kidney edema caused by the crystalloids we gave.
Absolutely. NS is given by medical peeps only by cultural habit. Most do not know the pH (zero SID due to chloride) of a solution they give by the buckets. RL is the best option I have available.
If you are involved in the early phase of resuscitation of a shocked patient, consider the downstream consequences of your fluid strategy that you give your patient that may give you a temporary comfort because they will look better in the short term.
Dr. Maitland and the FEAST study corroborates exactly this.
This is not to say that an aggressive and upfront resuscitation is not critical–it surely is. I’m saying resuscitate smarter, not wetter. Look for stop points for crystalloids–E/e’ ratios, consider PVPI, RV dilation/TAPSE, hepatic vein doppler, IVC dynamics, portal vein pulsatility, intra-renal venous Doppler patterns and renal resistive index. Fix the hemodynamics from an approach of the root of their problem, rather than pushing fluids for every hypotensive patient (whether you are taking care of them early, or late in the time frame of their illness). Fluids do have their place, but be careful and cognizant of their real down side. Look at your patient, think it through, and make the best actions for them.
Ok, now I don’t even get to have a punchline. Thanks Korbin!
So if this interests you, tune in to The Great Fluid Debate at H&R2018, and I look forward to meeting both Kylie and Korbin who will be in attendance and, I’m sure, putting us all on the spot!
And yes, there will be a POCUS workshop on portal and hepatic vein POCUS.
click here if you want to take part: H&R2018
cheers!
Philippe
POCUS & Venous Congestion – A Clinical Case Discussion with Rory Spiegel (@EMnerd_), #FOAMed, #FOAMus, #FOAMcc
Hi, so as a follow up to our earlier discussion, which can be found here, Rory and I discuss a recent case he had, which I think exemplifies well many of the clinical conundrums that are seen in fluid resuscitation, one being the general resistance of many to diurese patients who are still in shock on vasopressors, instead preferring to (hopefully) wait until shock resolution to de-resuscitate. But sometimes, it is exactly what they need, as some of this congestion may be, in fact, a cause of shock…
Here you go:
Love to hear opinions, so feel free to reach out.
For those who may be interested at learning some of these POCUS skills, check out H&R2018 (#Hres2018)!
cheers!
Philippe
Fluid Stop Points! More POCUS goodness from Korbin Haycock. #FOAMed, #FOAMcc
I am really enjoying this exchange, and I think it is in the true spirit of #FOAMed to foster these discussions, as we have the opportunity to combine and fine tune our understanding of a topic from several really bright people’s view and experience.
Korbin:
Jon-Emile, excellent points and insight. I should clarify a couple of my comments. To be specific, by “renal vein flow” I am referring to intra-renal venous flow. Apologies for my imprecision! Thanks for pointing that out.
Yes, a lot of these renal and portal Doppler patterns are surrogates of CVP. But I don’t think any of us would use CVP in isolation these days to make any decision what-so-ever on whether fluids were indicated in our patient.
Also, to clarify, I am not using intra-renal venous flow or renal resistive index as measures of non-fluid responsiveness. Rather, I use these measures as a stop point for attempting to solve the patient’s hemodynamic dysfunction with crystalloid regardless of whether or not my straight leg test tells me the patient is still fluid responsive.
And that is a key re-iteration to me. It is important to set these stop points and not only look at whether the cardiac output can be maximized. This has been tried. And failed. Let’s remember that sepsis is not inherently a disease of low flow. It isn’t cardiogenic or hypovolemic shock at the core.
My rationale for the strategy of using intra-renal Doppler, E/e’, and Lung US (now, I can include portal vein pulsatility) as a stop point for IVF administration is that I think the patient is best served to avoid iatrogenic edema of the upstream organs, primarily the lungs and the kidneys. These are the two organs (maybe you could put the endothelium in this category as well–glycocalyx being a whole other can of worms!) most easily damaged by the chase for optimizing every bit of fluid responsiveness. We have good evidence that getting wet lungs and swollen, congested kidneys is a bad thing, and we have these tools to hopefully warn us when we are pushing things too far.
Absolutely. And the whole glycocalyx is something to keep in mind, even if only to me mindful to disrupt it as little as possible.
Of course renal resistive index, intra-renal venous flow, portal vein pulsativity, and whatever else you like will have limitations and confounders. As long as you understand what can cause abnormalities with these tools, you can make an educated guess as to what’s going on. If our creatinine is off and our RRI is high, but intra-renal venous flow and portal vein flow is normal, perhaps the RRI is caused by something other than renal congestion, like ATN. If the portal vein is pulsatile, but the Doppler patterns of the hepatic vein, kidney and the heart look ok, maybe something else is wrong with the liver. But, if all our modalities are in agreement and pointing to congestion, we should perhaps believe that it’s congestion and stop the fluids.
That is an awesome approach to integrating RRI. I’ve been toying with it for the last couple of days, and much thanks to Korbin, I think that the limitations of RRI can be overcome by using the rest of our clinical and POCUS data.
It isn’t a hard technique, though in some patients getting a good signal can be tricky.
I think that the kidney, being an encapsulated organ, and the fact that much of our crystalloid ends up as interstitial edema, the kidney will develop sub-optimal flow patterns before CVP would cause congestion. The same is true regarding the lung, except that it’s just related to increased pulmonary permeability due to inflammation. Regardless, the idea is to save organs, and the earlier you can detect the problem, the sonner you can stop battering the more delicate organs with fluid.
As I think we have all mentioned, you really have to look at the whole picture, and put it together to tell the story of what is wrong, so we can logically and thoughtfully treat our patients.
I really appreciate this discussion. Thanks!
Thanks to Andre, Jon and Korbin for making this very educative for all!
Cheers
Philippe
ps don’t miss the POCUS Workshops on venous assessment at ![]() !!!
!!!
Jon-Emile (@heart_lung) chimes in on the whole portal vein POCUS! #FOAMcc, #FOAMed
When it comes to physiology, there`s no doubt that Jon is the man, so I was really curious about his take on all this, which, no surprise, is definitely worth sharing, just in case everyone doesn`t go read the comments.
Jon:
Wow; there is a lot to unpack here.
My first comment is that intra-renal venous flow [*not renal vein flow], hepatic vein flow, portal vein flow, etc, etc, etc [as well as IVC size and respiratory variation] are all ultrasonographic transductions of the central venous pressure …so I’ll give my boxed disclaimer that volume status and volume responsiveness cannot definitively and reliably obtained from this marker because the CVP is too complicated to make these physiological leaps.
Indeed. It is important to realize that, as Jon states below, that the angle for looking at the PV in this case is to assess congestion, rather than responsiveness or the ever-so-nebulous ‘status.’
Wait for it … volume tolerance and the CVP, is a bit more nuanced, i think. with a high CVP, you really have to ask yourself – **why** is the CVP elevated and go from there. if the CVP is elevated because of tamponade, its very different management from a high CVP from a massive PE or air-trapping versus a high CVP from volume overload.
Absolutely. Diuresing a pre- or full-fledged tamponade, PE or air-trapping could have disastrous consequences, i.e. PEA arrest!
There seems to be some confusion about *the renal vein* versus *intra-renal vein*. the lida trial is clear that it is intra-renal vein flow. i am not terribly familiar with *the renal vein flow, however, my hunch is that renal vein flow should always be biphasic [just as the jugular venous flow, SVC flow, IVC flow and hepatic vein flow are always biphasic] – that is a normal pattern close to the right atrium. normally the systolic inflow velocity is greater than the diastolic inflow velocity and there is fairly good data correlating reversal of systolic to diastolic venous flow ration to right atrial pressure [in the IVC and SVC].
Definitely the intra-renal vein should be the target here – not always easy in some patients, because the renal vein itself, especially the right (no crossover) really has an IVC pattern and won`t necessarily reflect the effect of intra-renal hypertension.
The pulsatility that evolves in the intra-renal vein as the CVP rises is beyond me, but the authors postulate that it has to do with the compliance of the vein at higher CVP and intra-renal interstitial pressure which makes some sense. But it is important to note that the compliance curves of an intra-renal vein and *the* renal vein are probably quite different.
Secondly, the pulsatility of the PV is a neat idea because of its relative ease of assessment. However, the pulsatility, presumably, is due to the PV encroaching the limits of its compliance curve – the PV, like the CVP – has an inflow and outflow pressure. It is highly likely that a pulsatile PV in a post-operative cardiac patient relates to an angry RV – but is this always true? What about the cirrhotic? What about differential partitioning of fluid into the splanchnic bed versus the lower body? What about differential expression of adreno-receptors between splanchnic arteries [beta and alpha] and splanchnic veins [mostly alpha]. My point is that there could be *other* inflow and outflow differentials that are affecting PV volume, compliance and therefore pulsatility that are not yet recognized. A cirrhotic on bomb dose phenylephrine/vasopressin may have their splanchnic venous volume recruited with blood expelled towards the liver, an engorged PV that is pulsatile – but is that RV failure? Is that a patient who needs to be decongested? I don’t know.
Thirdly, there are complex cardiac contributions to venous flow phase and vein pulsatility such as arrythmia – atrial compliance, etc. As the comment above notes – how might afib contribute to SVC or IVC venous inflow? It’s hard to know, but my hunch would be that afib itself would tend to reverse the normal S wave: D wave supremacy … that is, decrease the normal systolic inflow velocity relative to the diastolic inflow velocity. if the atrium is not emptied fully then its pressure with rise. if atrial pressure rises, when the atrium is pulled downward during ventricular systole, the S wave will be diminished. additionally, the more chronically dilated and poorly compliant the right atrium, the greater its pressure will be with the loss of atrial kick.
Fantastic points. Again, looking at POCUS metrics CANNOT BE DONE IN ISOLATION, from the rest of the POCUS and clinical data.
Lastly, the venous inflow pattern analysis approach to CVP estimation – i think – is better than IVC size and collapse because of how IVC size and collapse can also be affected by IAP, ITP/PEEP, etc. Because ITP affects systolic and diastolic inflow patterns similarly, that confound should be lessened. Nevertheless, as Dr. Denault mentions in the cases above – you have to treat the patient! This means integrating what the data is telling you in the patient in front of you. If in a certain clinical context the test results do not make sense, it’s probably a false positive or false negative test.
I dug up this gem from 30+ years ago. Excellent paper [https://www.ncbi.nlm.nih.gov/pubmed/3907280 – “Ultrasonic assessment of abdominal venous return. I. Effect of cardiac action and respiration on mean velocity pattern, cross-sectional area and flow in the inferior vena cava and portal vein”].
Ok that’s on my short reading list for the next 48h!
They show the venous inflow waveform for the IVC [presumably very similar to *the renal vein]; Afib *does* cause the S wave to become attenuated – so it would change the normal biphasic form to more of a monophasic form. In theory, giving a calcium channel blocker and slowing the patient down should improve this somewhat. They even have a brief discussion on portal vein pulsatility.
This venous inflow stuff is very interesting and potentially very applicable. @iceman tweeted out wave velocity patterns in the MCA during high ICP – indeed – an increase in ICP renders the flow more pulsatile and then there is loss of diastolic flow. Probably similar physiology for an intra-renal vein as intra-renal capsular pressure rises. A good sign that the kidney is under pressure!
Thank you Jon for some really excellent physiological points and the reminder that, in POCUS just as in clinical medicine, we cannot rely on one assessment, and that measure must be considered in the context of the factors affecting it. Otherwise, we are not truly tailoring our therapy to the patient, but only pretending to.
Don’t miss Jon and the POCUS workshops at  next april!
next april!
The Resuscitation Tracks 1: Portal Vein POCUS with Dr. Andre Denault. #FOAMed, #FOAMcc, #FOAMus
So this is one of the key discussions I wanted to have in my process of synthesizing my resuscitation algorithm. Dr. Denault is the one guy I’d call a mentor, and I think one of the rare and true clinician-scholar, who is just as comfortable being the anaesthetist/intensivist at the bedside of the crashing patient as he is being the keynote speaker in major conferences, or writing the textbooks that lead the field in acute care/perioperative TEE and critical care POCUS.
So to put some perspective to this discussion, back in 2014 I organized a resuscitation afternoon for internists with Andre and another awesome guy you probably all know, Haney Mallemat (@criticalcarenow). In a quick 15 minute discussion between talks, he shared with me the most recent of his discoveries, portal vein POCUS as a marker of right-sided failure/volume overload in his post-op cardiac patients, and how aggressively managing these resulted in much improved post-operative courses in terms of weaning, vasopressors and even delirium.
Interesting stuff.
So here you are:
So I’ll let you all ponder that and I would really like to hear comments and ideas. Sometime in the next few weeks I’ll be finalizing my resus algorithm – which will not be a recipe approach, as you might suspect if you have been following this blog, and will rely heavily on POCUS and the clinical exam.
cheers and thanks for reading and listening!
Don’t miss Andre running a POCUS workshop on PV/HV at  next april!
next april!
Philippe
A Discussion on Fluid Management Protocols with Rory Spiegel. #FOAMed, #FOAMcc, #POCUS
So Rory (@EMnerd) is in the process of working on a fluid resus protocol for Shock-Trauma, and asked me if we could have a chat about it, which I feel very honored for – and had a brief impostor syndrome crisis – but it’s always great to chat with people who are really bright, really physiological and after the same goal, to make patients better. Always a pleasure to chat with Rory, so here it is.
I really can’t wait to see their protocol, because I think this is a huge and complex endeavor, but has to be done. I will try to put pen to paper (probably really pixels to a screen but that doesn’t sound as good) and put what I try to do for fluid resus on a diagram of sorts.
Love to hear comments and questions.
PS please skip the first 30 seconds which are a technical blank… Ièm not tech saavy so can’t trim it!
cheers!
Philippe
A great comment by Dr. Korbin Haycock
One issue to consider is the degree of pulmonary vascular leakage. If, as in the case of sepsis, the pulmonary vasculature is more prone to the development of lung interstitial edema, lower LVEDP’s possibly will still result in as much lung wetness as higher LVEDP’s. Therefore, reliance of E/e’ ratios may not be the best measure of a fluid resuscitative endpoint in sepsis (and aren’t we really talking about sepsis resuscitation here?). I believe that it’s relatively clear that EVLW will adversely affect outcomes, but pushing for every bit of increased stroke volume/fluid responsiveness is less clear to be beneficial, even if it makes sense from a DO2/VO2 perspective (which may not be the real issue in sepsis anyway, as mitochondrial utilization of the DO2 provided may be the real problem, rather than DO2/VO2 balance). If the assumption is that the kidneys and lungs are the most delicate organs and most at risk to over aggressive fluid administration, and will impact mortality/LOS in the ICU, perhaps a combined strategy of attention to E/e’ ratios, development of B-lines, or the renal resistive index increasing would be a signal for a different strategy rather than fluids to increase venous return (i.e. switching from crystalloids to norepinephrine or vasopressin if the CO is elevated and will tolerate a minor ding from the increase in SVR). If any of those three variables indicate a problem, stop the fluids, switch to a vasopressor. If the issue is the CO rather than the SVR, use an inotrope instead. Of course RV/LV interactions as mentioned in the comments above must be considered. No point in giving fluids to an empty LV if the RV is failing–you’ll just congest the kidneys.
Bedside Ultrasound Case: Control the source. #POCUS #FOAMed, #FOAMcc, #FOAMus
So this morning a 65yr old man with shock and respiratory failure was admitted to the ICU, hypotensive on levophed and vasopressin, with a lactate over 10.
So, as usual, my first reflex was to reach for the probe to assess hemodynamics. He had been well resuscitated by a colleague, and the IVC was essentially normal, somewhere around 15 mm and still with some respiratory variation. However, scanning thru the liver, my colleague had noted a large hepatic lesion, which on CT scan (non-infused since patient had acute renal failure) the two radiologists argued whether it was solid, vascular or fluid filled.
Having the advantage of dynamic ultrasound, you can tell that there is some fluid motion within the structure, very suggestive of an abcess, especially in the context of severe septic shock:
So the next step was source control:
Pretty nasty. Pardon my french!
We got over 1.5 L of exceedingly foul pus.
Within a couple of hours the lactate dropped to 3 and the levophed was down by more than half.
I think this case illustrates once again, the power of POCUS in the hands of clinicians. While I am certain that the diagnosis would have been made without POCUS, it probably would have taken additional time as the radiologists themselves were debating its nature, and without POCUS, bedside drainage in the ICU would have been out of the question. That liter might still be in there tonight…
For those interested in how to integrate POCUS in their daily rounds, I think I put together a fair bit of clinical know-how and tips in this little handbook.
Cheers!
Philippe